I.
The duration of infectiousness of individuals infected with SARS-CoV-2 - PubMed (nih.gov)
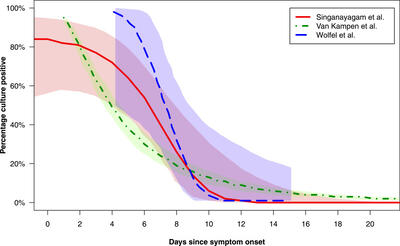
Depending on the study- 1. Singanayagam et al, 2. Van Kampen et al, [green interrupted line- most favorable to CDC still reveals 30-35% individuals could still be infectious. 3. Wolfel et al. Bothe Study #1 and #3 suggest longer duration of infectious. This justified testing atleast with two antigen tests on day 3 and 5 to see if the person is infectious and must increase the duration of isolation. Report #2 from the President of the AMA and Report #3 provides a detailed discussion on the duration of infectiousness and the useful role for two antigen tests to determine Not if one is Infected but on the Day of isolation is the person infectious. The CDC did NOT indicate this caveat the authors of the preprint study introduced in the report. If confirmed, this is a Travesty. The researchers found that community-based self-isolation strategies can reduce the infectious days during which the community is exposed to the worker to near-nil if release follows two successive days of negative tests, irrespective of when testing is resumed after the first positive test.
II.
COVID live updates: American Medical Association criticizes CDC's new guidance | WPHM
COVID live updates: American Medical Association criticizes CDC's new guidance
January 6, 2022 ABC News 0 Comments

Eric Lee/Bloomberg via Getty Images
(NEW YORK) — As the COVID-19 pandemic has swept the globe, more than 5.4 million people have died from the disease worldwide, including over 832,000 Americans, according to real-time data compiled by Johns Hopkins University’s Center for Systems Science and Engineering.
About 62.3% of the population in the United States is fully vaccinated against COVID-19, according to data from the Centers for Disease Control and Prevention.
Here’s how the news is developing. All times Eastern:
Jan 06, 4:05 am
American Medical Association criticizes CDC’s new guidance
The American Medical Association, the nation’s largest association of physicians, has criticized the Centers for Disease Control and Prevention’s new quarantine and isolation guidance for COVID-19, saying the recommendations “are risking further spread of the virus.”
The CDC updated its guidelines on Dec. 27, saying asymptomatic people who test positive for COVID-19 should self-isolate for five days rather than 10.
“The American people should be able to count on the Centers for Disease Control and Prevention (CDC) for timely, accurate, clear guidance to protect themselves, their loved ones, and their communities. Instead, the new recommendations on quarantine and isolation are not only confusing, but are risking further spread of the virus,” the American Medical Association’s president, Dr. Gerald E. Harmon, said in a statement Wednesday night.
Harmon referenced data cited by the CDC in its rationale for shortening the isolation period, which estimates 31% of people remain infectious five days after a positive COVID-19 test, suggesting that data proves thousands of Americans could return to their lives while still infected.
“With hundreds of thousands of new cases daily and more than a million positive reported cases on January 3, tens of thousands — potentially hundreds of thousands of people — could return to work and school infectious if they follow the CDC’s new guidance on ending isolation after five days without a negative test,” Harmon said. “Physicians are concerned that these recommendations put our patients at risk and could further overwhelm our health care system.”
Harmon said a negative COVID-19 test should be required for ending isolation after a positive test, as reentering society without knowing whether an individual is still positive ultimately risks further transmission of the virus.
Although test availability remains an issue nationwide, Harmon also called on the Biden administration to ramp up production and distribution of tests, adding that “a dearth of tests at the moment does not justify omitting a testing requirement to exit a now shortened isolation.”
III.
Model suggests feasibility of shorter COVID-19 isolation period with minimal risk (news-medical.net)
Model suggests feasibility of shorter COVID-19 isolation period with minimal risk
 By Dr. Liji Thomas, MD Jan 7 2022Reviewed by Danielle Ellis, B.Sc.
By Dr. Liji Thomas, MD Jan 7 2022Reviewed by Danielle Ellis, B.Sc.
The spread of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) during the ongoing coronavirus disease 2019 (COVID-19) pandemic has been impressive, and efforts to contain it have entailed extreme curtailment of social interactions, even for purposes of business or travel. With the emergence of the Omicron variant of the virus, things promise to become worse as it spreads even faster than the Delta, which itself was much more transmissible than the D614G variant.
The easy spread of the Omicron variant has led to the isolation of numerous healthcare and other frontline workers as they tested positive. The simultaneous removal of many key workers has placed great strain on the ability of organizations, especially healthcare facilities, to provide adequate staff for their requirements. This is particularly troublesome when it occurs when the trend of hospitalizations for moderate to severe disease is rising.
A new preprint reports the results of a model that sought to establish the minimum effective time to release workers in isolation, using a sliding scale based on lateral flow tests, in place of the fixed duration of self-isolation typically mandated in such situations.
Background
Omicron is considered an immune escape variant with high transmissibility compared to the immediately preceding Delta variant. As such, it is likely to drive an unprecedented wave of infections and hospitalizations, despite high levels of vaccination in several regions.
According to the policies in force, one effect of this will be the simultaneous loss of many workers who become infected and have to self-isolate. The typical period of self-isolation is ten days. The number of hospitalizations with Omicron will increase the risk of infection for hospital workers and other healthcare workers due to increased exposure. This will, in turn, increase the number of isolating workers and lead to an acute and detrimental shortage of workers.
A possible solution to this is to shorten the period of isolation for workers with a mild infection who feel able to work and test negative. This was explored in the current study, using either self-isolation alone or isolation with lateral flow tests to release. This approach aimed to monitor the extra days during which the worker was infectious.
The possibility of delaying the first test-to-release and reducing the number of consecutive negative tests required for release, was also assessed for its feasibility in low-resource settings.
In the current study, published on the medRxiv* preprint server, the researchers set up a model that included parameters such as the infectiousness of the individual, and lateral flow testing, in order to assess the effectiveness of test-to-release policies as compared to those with fixed-duration isolation mandates. The aim was to measure the excess days that they remained infectious, the days of unnecessary isolation that could be avoided with the former type of policy, and the tests used.
The researchers modeled populations of 10,000 each, with appropriate viral load trajectories and peak viral loads in the number of ribonucleic acid (RNA) copies/mL, to find an estimate of the chances of being infectious and testing positive per day. This was used to predict whether the individual is infectious and/or test-positive if the viral load is known for each day of infection.
Applying policy scenarios that had different isolation periods, of three, five, or seven days’ wait before beginning or resuming testing, they then examined the outcome in terms of how many days of isolation were avoided, vs. a 10-day isolation period, as well as the number of infectious days after release, and the number of tests required per 10,000 individuals, at one, two or three successive negative tests before release. They also looked at how it performed vs. a short period of isolation before release without testing.
Related Stories Levels
Using the same parameters for the Omicron variant as with earlier variants, such as the increase in viral load with time, the infectivity, and the chances of a positive test over time, allowed the researchers to examine the effect of a shorter proliferation phase.
These were used to predict the outcomes for vaccinated vs. unvaccinated individuals, assuming daily testing and isolation after they first test positive, thus becoming part of the modeled scenario. Symptom-based isolation policies were not covered.
What did the study show?
The researchers found that community-based self-isolation strategies can reduce the infectious days during which the community is exposed to the worker to near-nil if release follows two successive days of negative tests, irrespective of when testing is resumed after the first positive test.
There is a trade-off between the number of days saved in isolation by the earlier resumption of testing for release and the expense incurred in the greater number of tests required. If testing is resumed at three from the first positive test (the start of isolation), the number of infectious days is minimized. Still, the number of tests required before two successive negative tests are obtained will be higher.
In resource-scarce settings, a period of 5 or 7 days before resuming testing will achieve minimal transmission risk while using fewer tests, but at the cost of spending long periods out of work in isolation.
If the population is largely unvaccinated, the use of a mandatory 10-day isolation period would be superior, with fewer infectious days and fewer tests required to release. This is because the individual is expected to take a longer time to clear the virus, with a longer test positivity period than vaccinated individuals.
Suppose the proliferation phase with Omicron is shorter by half, irrespective of vaccination status. In that case, this will result in more rapid replication of the virus, with a higher viral load being achieved in fewer days. Hence, the patient is infectious earlier in the course of infection. In addition, however, this will result in individuals being infectious for shorter durations than other variants. This means a higher number of isolation days saved, with fewer infectious days and fewer tests to release.
What are the implications?
The results of this modeling study indicate that the 10-day self-isolation policies may be unnecessarily disruptive of the workforce or promote testing hesitancy for fear of forced lengthy absences from work. Already, some countries are altering their self-isolation guidelines due to this realization. The current model supports such changes by showing the risk of an infectious worker exposing the community to infection is low with a fixed-isolation period of only seven days.
[But in Absolute numbers it can be staggeringly high [R-Naught numbers are between 2-5-3] because on day 5, when isolation period is ended, 30 % of individuals are still infectious we need a testing regimen to detect whether person is infectious and not infected before they can leave isolation and return to their jobs. The AMA has taken this position: “With hundreds of thousands of new cases daily and more than a million positive reported cases on January 3, tens of thousands — potentially hundreds of thousands of people — could return to work and school infectious if they follow the CDC’s new guidance on ending isolation after five days without a negative test,” Harmon said. “Physicians are concerned that these recommendations put our patients at risk and could further overwhelm our health care system.”
Harmon said a negative COVID-19 test should be required for ending isolation after a positive test, as reentering society without knowing whether an individual is still positive ultimately risks further transmission of the virus. ”VM COVID live updates: American Medical Association criticizes CDC's new guidance | WPHM
If combined with test-to-release policies that involve beginning to test after three or five days, until two successive negative tests are obtained, this period maybe even less. Such strategies may be crucial in ensuring barely adequate staffing is available during this period of heavy demand in professions such as healthcare, despite a small increase in the risk.
The use of viral parameters from pre-Omicron days may affect the reliability of these predictions. Moreover, since some research suggests that lateral flow tests are more sensitive to the presence of the virus even at non-infectious viral loads, a 10-day isolation period may have to be shortened regardless of a positive test at this point, since the latter may not reflect true infectiousness.
Further, the effect of isolating from the onset of symptoms may further reduce the isolation time. These assumptions need to be tested and validated before being used as the basis of new policies. Keeping this in mind, however, the researchers suggest,
Based on a model of viral load kinetics, infectivity, and test sensitivity, shortening the isolation period for SARS-CoV-2 test positive individuals carries minimal risk which can be reduced further by requiring consecutive negative lateral flow tests to release.”
*Important notice
medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.
Journal reference:
- Quilty, B., Pulliam, J. and Pearson, C. (2022) "Test to release from isolation after testing positive for SARS-CoV-2". medRxiv. doi: 10.1101/2022.01.04.21268372. https://www.medrxiv.org/content/10.1101/2022.01.04.21268372v1
Posted in: Medical Science News | Medical Research News | Disease/Infection News
Tags: Coronavirus, covid-19, Healthcare, Hospital, Omicron, Pandemic, Proliferation, Research, Respiratory, Ribonucleic Acid, RNA, SARS, SARS-CoV-2, Severe Acute Respiratory, Severe Acute Respiratory Syndrome, Syndrome, Virus
IV. Test to release from isolation after testing positive for SARS-CoV-2. This is Original Study on which the shortened isolation periods was based. But this study specifically recommends screening for infectiousness with antigen tests. VM
View ORCID ProfileBilly J. Quilty, View ORCID ProfileJuliet R. C. Pulliam, View ORCID ProfileCarl A. B. Pearson
doi: https://doi.org/10.1101/2022.01.04.21268372
Summary
- The rapid spread and high transmissibility of the Omicron variant of SARS-CoV-2 is likely to lead to a significant number of key workers testing positive simultaneously.
- Under a policy of self-isolation after testing positive, this may lead to extreme staffing shortfalls at the same time as e.g. hospital admissions are peaking.
- Using a model of individual infectiousness and testing with lateral flow tests (LFT), we evaluate test-to-release policies against conventional fixed-duration isolation policies in terms of excess days of infectiousness, days saved, and tests used.
- We find that the number of infectious days in the community can be reduced to almost zero by requiring at least 2 consecutive days of negative tests, regardless of the number of days’ wait until testing again after initially testing positive.
- On average, a policy of fewer days’ wait until initiating testing (e.g 3 or 5 days) results in more days saved vs. a 10-day isolation period, but also requires a greater number of tests.
- Due to a lack of specific data on viral load progression, infectivity, and likelihood of testing positive by LFT over the course of an Omicron infection, we assume the same parameters as for pre-Omicron variants and explore the impact of a possible shorter proliferation phase.
Competing Interest Statement
The authors have declared no competing interest.
V. A.
The Situation Room – Wolf Blitzer Transcript 6PM, 01 05 22
From 6:20 to 6:25 PM Wolf Blitzer interviewed Dr. Sanjay Gupta, Chief Medical Correspondent-CNN and Dr. Gerald Harmon, MD., President of the AMA. I have posted the official critical response of the AMA to the CDC Guidelines from Dec 27 2021.
Let's bring in our Chief Medical Correspondent Dr. Sanjay Gupta, as well as president of the American Medical Association, Dr. Gerald Harmon. Doctor, thank you, both of you, for joining me.
Sanjay, let me start with the breaking news, CDC advisers just a little while ago recommending expanding boosters for Americans as young as 12 years old. Sanjay, how significant is this development?
DR. SANJAY GUPTA, CNN CHIEF MEDICAL CORRESPONDENT: Well, on a personal note, I have two children that fall into that category, so they will be getting their booster shots. My older daughter already got hers. She is 16. So, I think it will make a difference for people who qualify.
Here is the issue, Wolf. I think we are talking overall in the country about 5 percent of the population, and of that 5 percent -- these are people between the ages of 12 and 15 -- only about half have already gotten their first two shots. So, you know, it is a relatively small percentage that we're talking about that are going to be impacted by this.
So, it is good for them, you know, to be able to get this added protection, but the real problem still, Wolf, whether it is children or adults is still primarily the unvaccinated. This is giving another layer of protection to people who already have pretty good protection. That's good. That's important, but when you look at the numbers on the right side of the screen in terms of the hospitalizations in particular, those are primarily people who are unvaccinated completely, Wolf.
BLITZER: Yes, that's absolutely true. Dr. Harmon, let me ask you about the new isolation guidance we have received from the CDC. You say it is, and I am quoting you now, confusing and counterproductive. So, what are they getting wrong?
DR. GERALD HARMON, PRESIDENT, AMERICAN MEDICAL ASSOCIATION: Well, it is a good point, Wolf. And to your point, what we at the AMA have is a concern that if you are going to end a period of isolation after an active COVID infection, it would be nice to have, in fact, we would recommend a valid negative COVID test, an antigen test, a rapid test in order to ensure that you are no longer shedding the virus, no longer transmissible and you tend to validate you are not contagious before you go back into your workforce, your family and potentially spread the virus more.
BLITZER: Yes, I think that's significant as well. Sanjay, you have a new essay on this issue coming out soon on cnn.com about how the CDC is missing the mark on these guidelines. What do you see as the main failure here?
01 05 22, 3:23 PM PST- Comments on the Graph illustrating Duration of Infectiousness.
GUPTA: Well, first of all, I completely agree with Dr. Harmon here on the fact that this is confusing. I mean, there's a couple of things. I don't know if we have this graph, Wolf. I want to show you one of the studies they actually looked at to determine how contagious are you on what day after you have been diagnosed with COVID.
So, we're talking about day five here. That's when they say, look, day five, you could potentially be ending your isolation. Well, we know on day five, 31 percent, roughly a third of people are still contagious. So, if those people, as the doctor mentioned, aren't getting tested, that's potentially putting a lot of people out into the public that could potentially transmit the virus. So, the fact that you don't have testing, the fact that there's still a significant percentage that could be contagious at that point I think is of concern.
And I would add to that, Wolf, that the masks issue, you know, we've talked about this a lot, but CDC is still saying, you know, three-ply cloth masks are okay. Omicron spreads very easily from person to person, and being able to have these masks, N-95, or KN-95 masks, which are more plentifully available now, I think, is really important now. If you are going to wear a mask, which you should, you should wear a good mask. So, those are three areas where I think the message could be a lot clearer and more effective.
BLITZER: Yes. And that's also an excellent point.
Dr. Harmon, you say the CDC's ambiguous guidance could allow this virus to spread further. Just how real are the consequences of this messaging failure?
HARMON: Well, this isn't an AMA versus a CDC issue. From what you heard to Dr. Gupta's point, what we're after is if you have a COVID infection, we want to make sure before you resume your day-to-day activities and spread this virus, and it is a highly transmissible virus with consequences, it would be nice to have a validating negative test to know you are safe and you have a substantially lowered risk of spreading the virus.
[18:25:01]
If you put these folks back into the workplace -- and I understand the forces that are driving this, we want folks to get back to a sense of normalcy, we want them to be in the workforce, we want them to be in the health care workforce. Goodness, we have enough shortages across the spectrum. But when they go back, we don't want them to spread the virus and then further impact the negative workforce issue. Dr. Gerald Harmon, MD
BLITZER: Dr. Gerald Harmon and Dr. Sanjay Gupta, to both doctors, thank you very, very much for all you are doing. Thanks very much for joining us.
V. B.
This is actual Videotape of the Interview: The Interview with Drs Gupta and Harmon, start around 3:21 pm PST on 01 05 22. The data that Dr. Gupta speaks about in the transcript can be seen at 3:21PST through 3:25PM PST. At 3:23 PM PST Dr. Sanjay Gupta talks about this graph on the duration of Infectiousness that is not displayed for some reason on the screen. The text below the Video and on the Transcript above Dr Gupta’s comments are clearly stated. The Videotape is quite helpful along with the Transcript. I have made comments on the previous Item #4
Velandy Manohar, MD.

